Ivcd symptoms5/29/2023  :max_bytes(150000):strip_icc()/Bundle-Branch-Block-58960e843df78caebceafb79.jpg)
Of the overall sample, 1,240 patients (5.6%) had QRS prolongation and broke down as follows: Outcomes measured were all-cause and cardiovascular mortality, with HF hospitalization a secondary outcome. Twenty-three percent had established cardiovascular disease, and arthritis type was adjusted for in multivariate analysis. Mean age was 63 years, and 64% of patients were female. Subjects without these findings were categorized as non-LBBB-predominant (O-IVCD).Īverage follow-up was 34 ± 13 months. IVCD with LBBB-predominant features (L-IVCD) required the following ECG findings: (1) lead V1 net negative (2) lead V1 without terminal positivity and (3) lead I net positive. The researchers devised a first-of-kind subclassification scheme for IVCD. IVCD was defined overall as QRS 101 to 120 ms irrespective of morphology, or as QRS > 120 ms not identifiable as BBB. 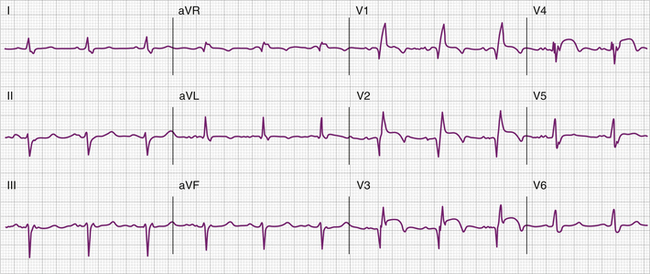
LBBB and RBBB were identified according to standard definitions (QRS duration > 120 ms). The present study categorized QRS duration as narrow (≤ 100 ms) or prolonged (> 100 ms), with prolongation further classified into LBBB, right bundle branch block (RBBB) and intraventricular conduction delay (IVCD). The Cleveland Clinic Coordinating Center for Clinical Research ( C5Research) adjudicated all-cause and cardiovascular mortality as well as heart failure (HF) hospitalizations and ECG results. Patients enrolled underwent a baseline 12-lead ECG. PRECISION found in 2016 that celecoxib does not confer excess cardiovascular risk and is associated with fewer cardiovascular adverse events compared with both naproxen and ibuprofen in patients with rheumatoid arthritis or osteoarthritis. This post hoc analysis included 22,607 (94%) of the randomized, double-blind, multicenter PRECISION trial’s 24,081 patients. “Our analysis makes a strong case for recognizing any type of delayed LV conduction among well-recognized cardiovascular risk factors, and thus changing how we think about overall cardiovascular health.” New subclassification scheme for intraventricular conduction delay “We have long established that delayed left ventricular conduction in the form of left bundle branch block confers markedly increased risk for cardiovascular and overall mortality in patients,” says the study’s corresponding and senior author, Daniel Cantillon, MD, of Cleveland Clinic’s Section of Electrophysiology and Pacing. We do not endorse non-Cleveland Clinic products or services Policy Advertising on our site helps support our mission. Cleveland Clinic is a non-profit academic medical center. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
